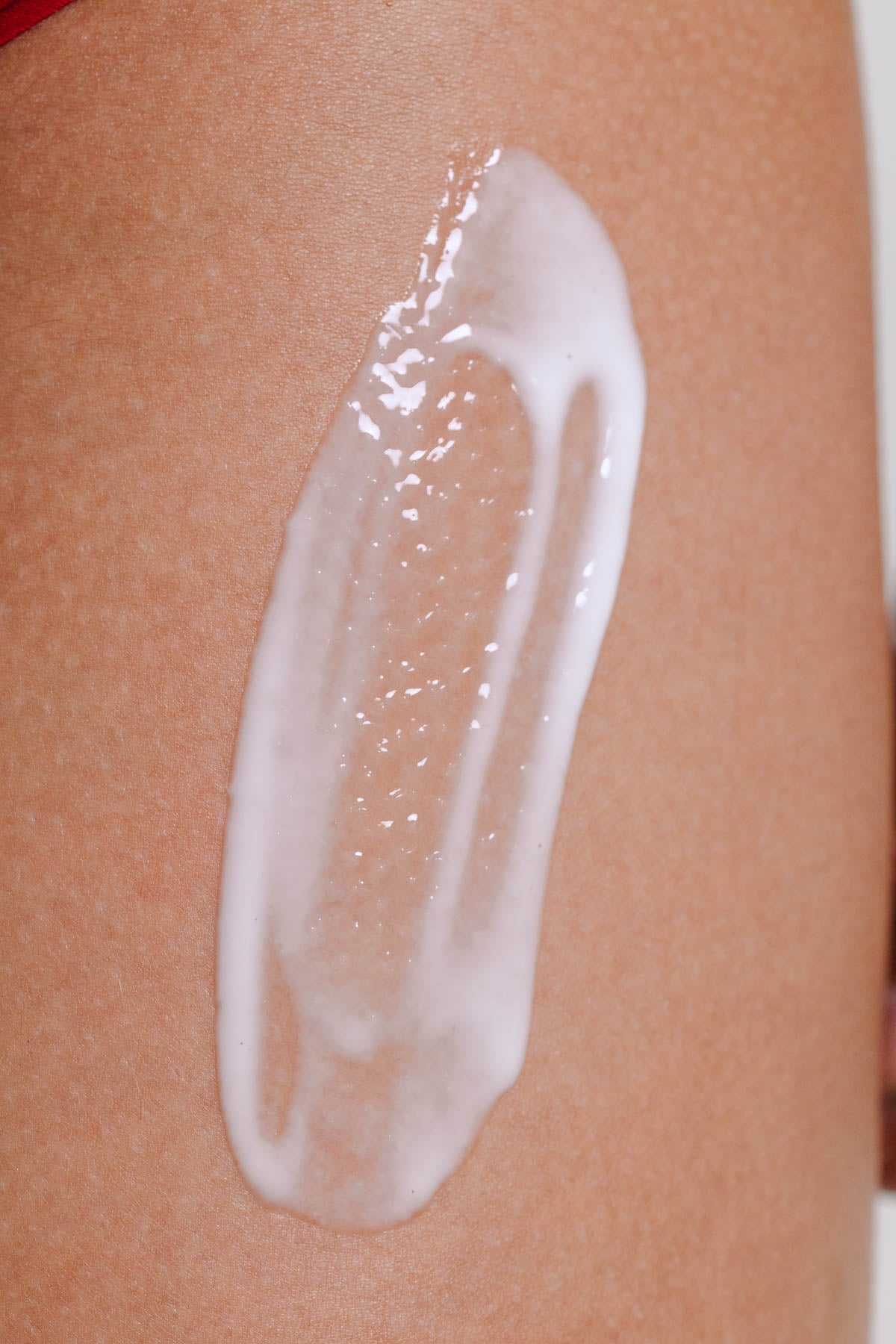
Keratosis pilaris is a skin condition that many people live with for years without getting a clear explanation for. Often referred to as strawberry skin, chicken skin or simply KP, it shows up as small, rough bumps (most commonly on the arms, thighs, and buttocks). While keratosis pilaris is harmless, it can affect how skin looks and feels, which is why so many people search for ways to improve it.
This guide breaks down what keratosis pilaris actually is, what causes it, and how thoughtful skincare habits may help soften and smooth the skin over time.
What Is Keratosis Pilaris?
Keratosis pilaris is a very common skin condition caused by a buildup of keratin, a protein naturally found in the skin. In KP-prone skin, excess keratin blocks hair follicles. This leads to small, raised bumps that may appear red, flesh-toned, or slightly darker than the surrounding skin.
These bumps are not pimples, and they’re not caused by dirt or bacteria. Treating keratosis pilaris like acne often makes it more noticeable. This means harsh cleansers, drying treatments, or aggressive scrubs should be avoided.
Keratosis pilaris is not contagious and doesn’t pose any health risk. For most adults, it’s a texture and appearance concern rather than a medical issue.
Common Areas Where KP Appears
In adults, keratosis pilaris most commonly affects:
-
Upper arms
-
Thighs
-
Buttocks
These areas often feel dry, rough, or uneven, even when moisturized regularly.
Keratosis Pilaris vs. Strawberry Skin
The term 'strawberry skin' is often used to describe the dotted appearance of visible follicles, especially after shaving. While strawberry skin can have multiple causes, keratosis pilaris is one of the most common, particularly when bumps are persistent and have a rough, sandpaper-like texture.
Not all strawberry skin is keratosis pilaris, but many cases of KP are described that way.
What Causes Keratosis Pilaris?
There isn’t one cause of keratosis pilaris, but several factors are known to play a role.
Genetics
Keratosis pilaris often runs in families. If a parent or sibling has KP, you’re more likely to experience it as well.
Keratin Buildup
The main sign of KP is excess keratin blocking the hair follicle. Why this happens in some people and not others isn’t fully understood, but it’s not related to hygiene or skincare mistakes.
Dry or Dehydrated Skin
KP tends to be more visible when the skin is dry. Many people notice flare-ups in colder weather or during seasonal changes when skin barrier function is weakened.
Sensitive or Reactive Skin
Those with sensitive skin, eczema-prone skin, or a history of a damaged skin barrier often experience keratosis pilaris alongside general dryness or irritation.
Is Keratosis Pilaris Treatable?
There is currently no known cure for keratosis pilaris. Any product or routine that claims to remove it permanently it should be approached with caution.
That said, many people see meaningful improvements in skin texture and appearance through consistent, gentle care. When treating keratosis pilaris, the main goals should be to:
-
Minimize the appearance of bumps
-
Smooth rough texture
-
Support overall skin comfort and hydration
Progress takes time, and results vary depending on skin type, sensitivity, and consistency.
How to Help Keratosis Pilaris Without Irritating the Skin
The most effective way to reduce the appearance of keratosis pilaris is to follow a skincare routine that prioritize barrier support and gentle exfoliation rather than harsh “fixes”.
1. Use Gentle Chemical Exfoliation
Physical scrubs with rough particles can irritate KP-prone skin and worsen redness. Instead, many people find better results with chemical exfoliants that work more evenly across the skin.
Ingredients commonly associated with helping keratosis pilaris include:
-
AHAs (alpha hydroxy acids), such as lactic or glycolic acid, which help loosen dead skin on the surface
-
BHAs (beta hydroxy acids), such as salicylic acid, which can penetrate into the follicle
A pre-shower exfoliating formula like Soft-Touch, which combines AHA 30% + BHA 2%, is designed to be used as a mask, rather than aggressively rubbed onto the skin. Used once or twice a week and followed by proper hydration, this type of exfoliation may help improve skin smoothness over time. While it isn’t a medical treatment, customer reviews suggest it’s a helpful addition to their KP routine.
2. Moisturize With Barrier Support in Mind
Moisturizing is often forgotten in keratosis pilaris routines, but it is essential. KP-prone skin isn’t just rough—it’s often dehydrated and has a weakened skin barrier.
Instead of using thick lotions, many people benefit from moisturizers that:
-
Help the skin retain water
-
Support the skin barrier
-
Improve overall texture without feeling heavy
This is where texture and formulation matter. A lightweight serum-lotion hybrid like Summer Skin can be well-suited to keratosis pilaris-prone areas. Designed to deliver hydration alongside active ingredients that support barrier function, it absorbs easily while keeping the skin moisturized.
If applied consistently, especially after exfoliation, this type of formula may help reduce the dry, tight feeling that often makes KP look more noticeable. While it won’t “treat” keratosis pilaris, supporting hydration and barrier health can make a visible difference in how skin looks and feels over time.
3. Apply Moisturizer Strategically
For best results:
-
Apply moisturizer while skin is still slightly damp
-
Focus on consistency rather than switching products frequently
-
Avoid fragranced or heavily drying formulas if skin is sensitive
Hydration doesn’t remove keratin buildup on its own, but it can help soften texture and reduce irritation.
4. Be Mindful With Hair Removal
Shaving can make strawberry skin more noticeable, especially if follicles are already blocked.
If shaving KP-prone areas:
-
Use a sharp, clean razor
-
Shave at the end of a shower when skin is softened
-
Avoid dry shaving or repeated passes over the same area
Some people find that reducing shaving frequency helps minimize irritation and visible dots.
5. Avoid Over-Exfoliating
More exfoliation does not equal faster results. Overdoing it can damage the skin barrier and lead to increased redness or sensitivity.
For most people, exfoliating once or twice a week is enough. Improvement tends to come from consistency and balance, rather than exfoliating more often or using harsher treatments.
Ingredients Often Used in Keratosis Pilaris Routines
While no ingredient guarantees results, the following are commonly included in routines designed to help manage keratosis pilaris:
-
AHAs (glycolic acid, lactic acid)
-
BHAs (salicylic acid)
-
Urea
-
Glycerin
-
Ceramides
Products made for sensitive skin are usually easier on the skin, especially if your KP comes with dryness or easily irritated skin.
How Long Does It Take to See Results?
Keratosis pilaris rarely changes overnight. Many people notice subtle improvements in skin softness and smoothness after several weeks of following a routine.
It’s also normal for KP to fluctuate due to:
-
Weather changes
-
Hormonal shifts
-
Stress
-
Changes in routine
Flare-ups don’t always mean your routine isn’t working; they’re often part of the process.
When to Consider Professional Advice
If keratosis pilaris is accompanied by ongoing redness, discomfort, or inflammation, a dermatologist can help confirm the diagnosis and rule out other skin conditions.
For most adults, KP is a cosmetic concern that can be managed with supportive, at-home care.
A More Balanced Approach to Keratosis Pilaris
Keratosis pilaris is extremely common, yet it’s often framed as something that needs to be aggressively “fixed”. In reality, KP-prone skin usually responds better to patience, consistency, and barrier-focused routines.
Pairing gentle exfoliation from products like Soft-Touch with hydration-focused formulas such as Summer Skin can help skin feel smoother and more comfortable over time, without pushing it past its limits.
Keratosis pilaris doesn’t define skin health, and it doesn’t need to disappear for skin to be cared for well. Sometimes, the most meaningful changes come from working with the skin rather than against it.